Rather than targeting the typical rogue proteins associated with dementia, scientists say that—for the very first time—they have reversed dementia in mice with a drug that reduces inflammation.
Up until now, most dementia treatments have targeted the amyloid plaques that are found in people with Alzheimer’s disease. However, the latest study published in Science Translational Medicine suggests targeting inflammation in the brain might stop it in its tracks.
In experiments conducted at the University of California, Berkeley, senile mice were significantly better at learning new tasks, and became almost as adept as those half their age.
Experts are “optimistic” that it will work in humans and possibly lead to a cure for the devastating neurological condition. Not only that, they hope that any drugs developed with their strategy can also help brains recover from strokes, concussions, or traumatic brain injuries.
The successful treatment in mice supports a growing body of research which says that our blood-brain barriers begin to leak as we get older. This is the filtration system that blocks infectious organisms, letting in chemicals that destroy neurons.
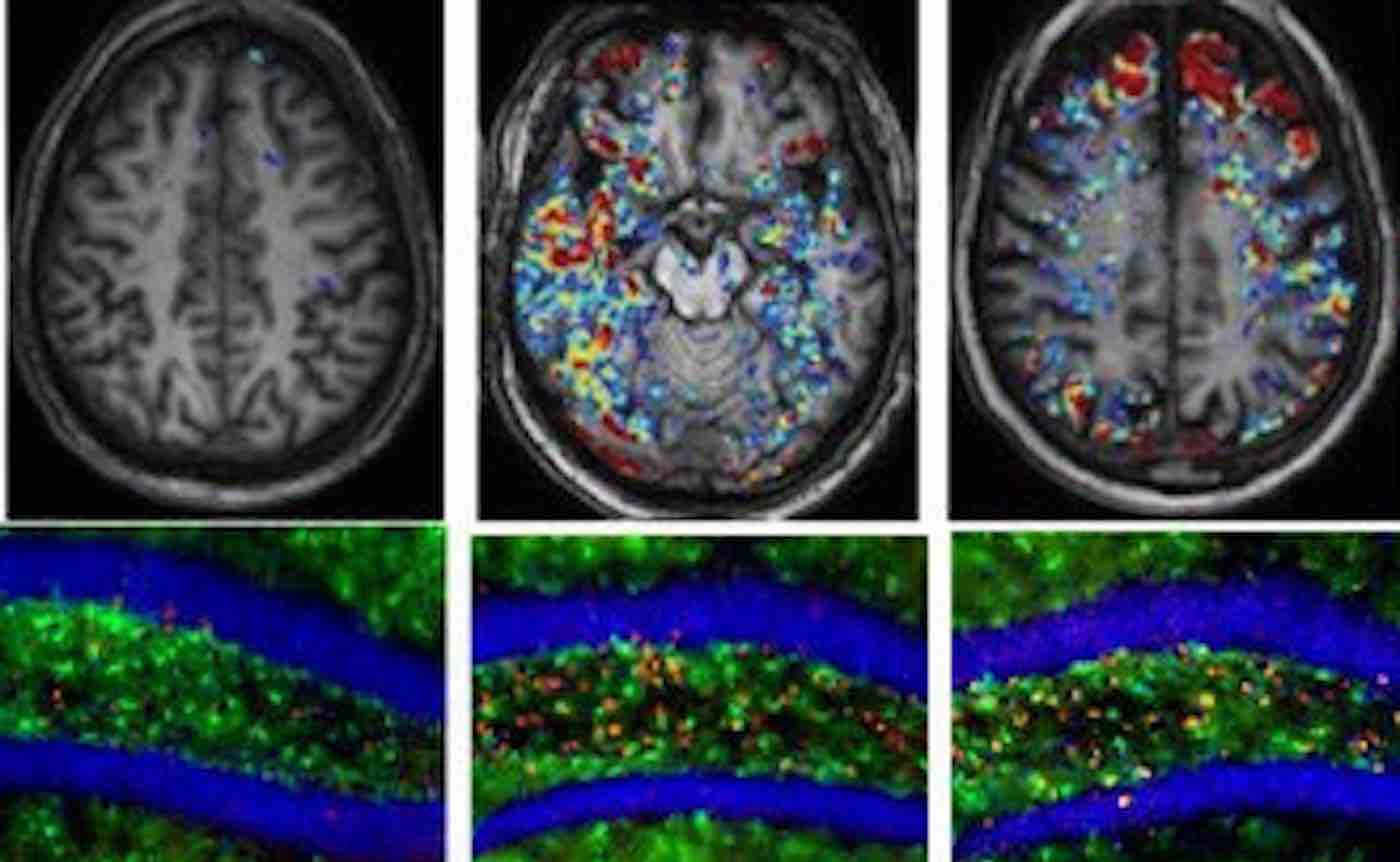
Previous MRI (magnetic resonance imaging) scans by study co-author Professor Alon Friedman have found that the barrier breaks down in nearly 60% of people by the age of 70.
CHECK OUT: New Research Links Five Simple Lifestyle Choices to a 60% Reduced Risk of Developing Alzheimer’s
Experiments in mice showed this causes an inflammatory fog that alters the brain’s rhythms, causing tiny seizure-like events. This leads to momentary lapses in the hippocampus that controls memory—shedding fresh light on the symptoms of dementia and other degenerative brain diseases.
“We tend to think about the aged brain in the same way we think about neuro-degeneration,” said senior author Professor Daniela Kaufer of the University of California, Berkeley. “Age involves loss of function and dead cells. But our new data tell a different story about why the aged brain is not functioning well.
“It is because of this ‘fog’ of inflammatory load. But when you remove that inflammatory fog, within days, the aged brain acts like a young brain,” he added. “It is a really, really optimistic finding, in terms of the capacity for plasticity that exists in the brain. We can reverse brain aging.”
MORE: Another Study Shows How Flickering Lights Can Slow (And Maybe Even Reverse) Alzheimer’s Symptoms
Scans called EEGs (electroencephalograms) revealed similar brain wave disruption in humans with Alzheimer’s, mild cognitive impairment (MCI) and epilepsy.
It means leaky barriers and abnormal brain rhythms detectable by MRI and EEG scans, respectively, can be used to flag people with dementia—as well as signal an intervention opportunity using a drug to slow or reverse the disease.
The drug, called IPW, blocks a gene known as TGF-β that fuels the inflammation triggering blood protein albumin.
RELATED: Be Sure and Floss! Researchers Say Good Dental Health ‘Substantially’ Decreases Risk of Alzheimer’s
“We now have two biomarkers that tell you exactly where the blood-brain barrier is leaking, so you can select patients for treatment and make decisions about how long you give the drug,” said Professor Kaufer. “You can follow them, and when the blood-brain barrier is healed, you no longer need the drug.”
When they gave the drug to mice in doses that lowered the gene’s activity, their brains looked younger; there was less inflammation and improved brain waves as well as reduced seizure susceptibility. The mice also navigated a maze and learned spatial tasks similarly to a young mouse.
In an analysis of brain tissue from humans, Professor Kaufer found evidence of albumin in aged brains and increased neuro-inflammation and TGF-β production.
Prof Friedman, of Ben-Gurion University of the Negev in Israel, developed a scanning technique called DCE (dynamic contrast-enhanced)—a special type of MRI. This detected more leakage in the blood-brain barrier of people with greater cognitive decline.
WATCH: Inventor Makes ‘Music Memory Box’ So Dementia Patients Can Reconnect With Their Loved Ones
Altogether, the evidence points to a disfunction in the brain’s blood filtration system as one of the earliest triggers of neurological aging, said Kaufer.
Her team have now started a company to develop a drug to heal the blood-brain barrier for clinical treatment—and it may eventually help older adults with dementia or Alzheimer’s disease who have demonstrated leakage of the blood-brain barrier.
“We got to this through this back door; we started with questions about plasticity having to do with the blood-brain barrier, traumatic brain injury and how epilepsy develops,” said Kaufer. “But after we’d learned a lot about the mechanisms, we started thinking that maybe in aging, it is the same story. This is new biology, a completely new angle on why neurological function deteriorates as the brain ages.”
Currently, the only drugs for dementia or Alzheimer’s treat the symptoms and not the cause. This new drug, however, opens the door to changing just that.
Cure Your Friends Of Negativity By Sharing The Good News To Social Media…