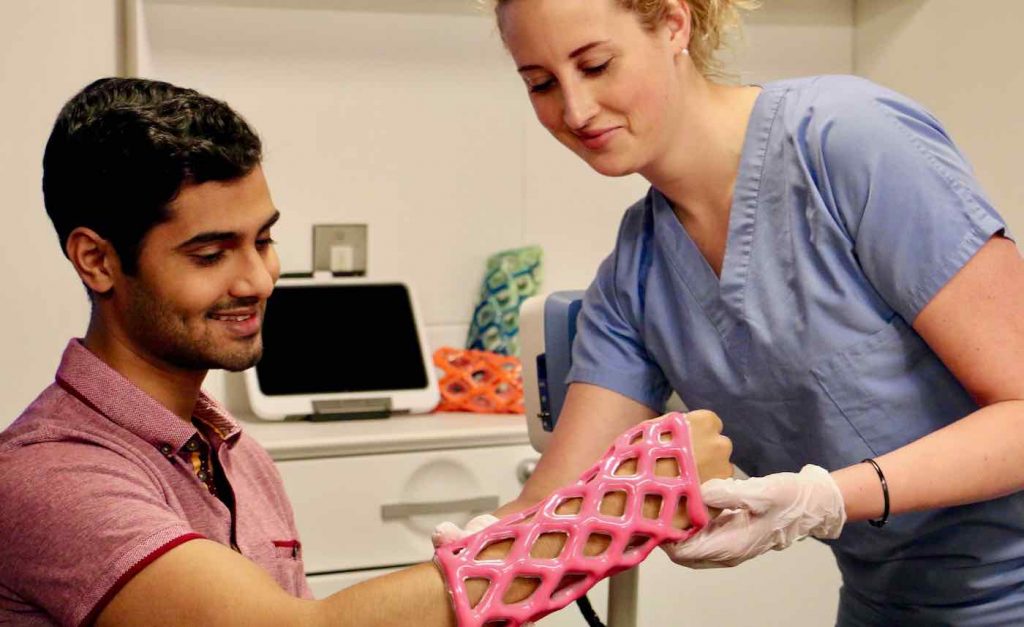
Engineers in Chicago have designed a futuristic sleeve that could make itchy, foul-smelling, uncomfortable plaster casts a thing of the past.
Their startup company, Cast21, has created a waterproof, lightweight, and breathable alternative that can be worn while bathing, exercising, and even swimming in the ocean.
The patented design is constructed from a wide mesh sleeve filled with two liquid resins which are molded into the correct position for each patient—and it is even available in a range of vibrant colors.
CHECK OUT: People With Diabetes May One Day Be Monitoring Glucose With an Earring
Patients sporting traditional plaster or fiberglass casts are unable to clean underneath the molded brace, making the skin susceptible to rot and infection. When it is time to remove the hardened bandages, wearers are also forced to watch a doctor remove their casts using a circular saw.
“The majority of fractures happen in children, adolescents and the elderly,” said Cast21’s VP of engineering Veronica Hogg. “Those saws are very loud and all this debris flies off and it’s very messy, it can be extremely frightening. The cast saw also presents a risk of burns to the patient.
“Our product does not require that at all. It’s designed so that a physician can take clinical shears, snip through the tabs and pull it open easily. It was designed to completely eliminate the use of a cast saw and make the healing process far more pleasant for the patient.”

The device is also faster to apply than traditional casts. Physicians start by measuring the damaged limb using a flexible measuring tape. Once they’ve selected the correct size, they slide a flexible, slightly padded, sleeve onto their patient’s arm.
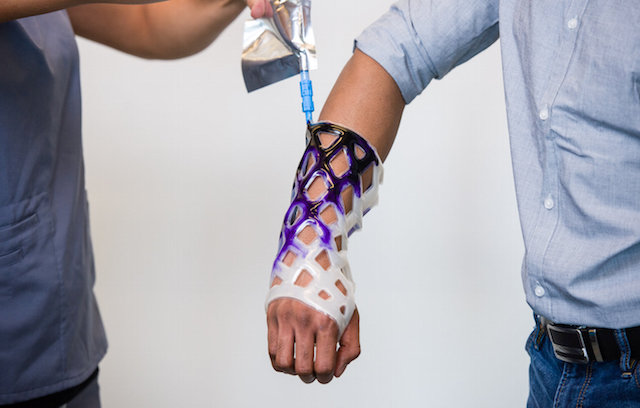
Using a patented liquid pack, the physician then mixes a duo of liquid resins and pours them into the empty sleeve through a valved nozzle.
After the sleeve is full, it takes three minutes for the liquid to turn into a malleable gel. The doctor then molds the product to fit the patient’s limb, and waits an additional five to seven minutes for it to completely harden.
“Another bonus is that no electricity or water is needed to apply our cast, so it’s very portable,” says the 30-year-old engineer.
There is reportedly no pain associated with the device’s hardening, and the exothermic heat it produces could even be beneficial.
“It feels soothing,” she added. “It reaches about the same temperature as a hot tub.”
While Cast21 hopes to make a splash in the field of orthopedic technology, the innovation is still a work in progress. So far the company only has a forearm model designed in a medium size—but they hope to expand their sizing and create casts for the lower legs in the near future.
“The idea is to prove that this technology works… right now, we are past the prototype stage and have a fully functioning model in place for the forearm,” said Hogg. “We hope that this technology can span across the entire body. We are looking forward to having a lower limb model for ankle fractures soon.

“We have this radical notion that you can enjoy your healing experience. You don’t need to be restrained from daily activities. I’m from Colorado and I like to go hiking, and the equipment needed to administer our cast is so small and lightweight that hikers and climbers could carry it with them in their backpacks (as a first aid kit).
“It also has potential for use in the military and for at-home first aid. 3D printed casts can be very expensive, and the turnaround time is very slow. Our design is almost instant and very portable.”
Waterproof, 3D-printed casts are already on the market around the US and Europe, but they can cost hundreds of dollars, and patients can be left waiting days or weeks for the cast to be printed and delivered to them. There is currently no price point associated with Cast21’s product, but the aim is to make it as accessible as possible.

“We want it to be competitive, and reachable to a large population. We don’t want this to be a luxury product. We are still conducting research in price sensitivity, and the final cost to the patients will be depending on their insurance and doctor.
“Right now, we can treat what’s known as ‘distal radial fractures’ or DR fractures; that’s a catch-all term for any fracture of the radius that occurs close to the wrist.
“We are hoping, with more data and feedback from physicians, that they would feel comfortable using this technology after a surgery was required. We are interested in expanding the pilot use of our product in clinics. So we would love for anyone interested to reach out to us for more information.”
Whether you are a doctor or patient, use the Contact form at the bottom of the website’s homepage.

Treat Your Friends To The Intriguing News By Sharing It To Social Media…