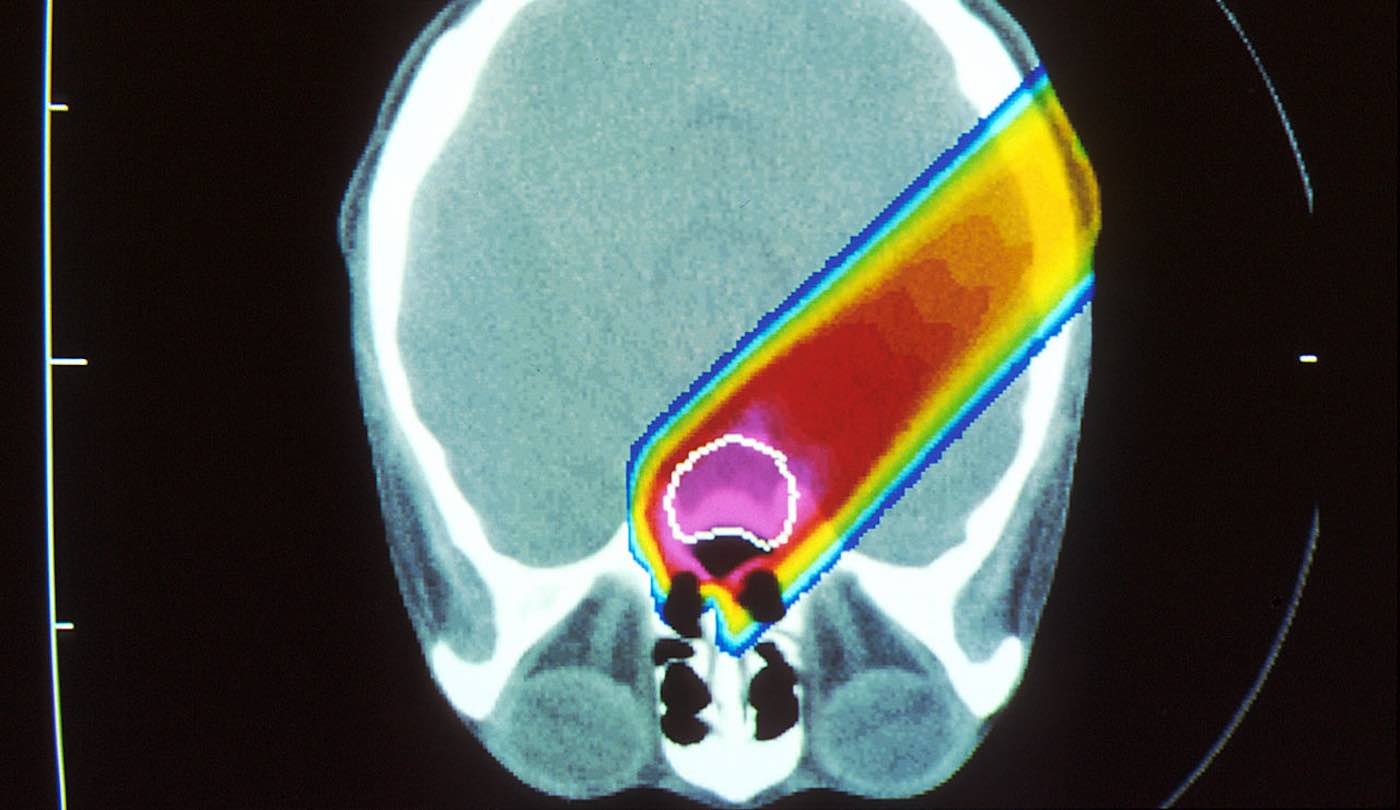
This exciting new study shows that “proton therapy” is a stunningly effective noninvasive treatment against high-risk childhood cancers – and it comes with minimal side effects.
Unlike traditional photon radiation using x-rays, proton radiation therapy (PRT) is a non-invasive, precise cancer treatment that uses a beam of protons moving at very high speeds to destroy the DNA of cancer cells, killing them and preventing them from multiplying.
Highly targeted, PRT has significant promise for treating tumors in very young children and may reduce radiation exposure to healthy, developing tissue that may result in lifelong impacts.
Researchers from Children’s Hospital of Philadelphia (CHOP) and the Perelman School of Medicine at the University of Pennsylvania analyzed the largest cohort to date of pediatric patients with high-risk neuroblastoma who were treated with proton radiation therapy.
Not only did they find that proton therapy was effective at reducing tumors, they also found that it demonstrated minimal toxicity to surrounding organs.
The study is published online in the International Journal of Radiation Oncology • Biology • Physics.
“These data are extremely encouraging and could be a game-changer for a number of reasons,” said lead author Christine Hill-Kayser, Chief of the Pediatric Radiation Oncology Service at Penn Medicine.
“Not only did we observe excellent outcomes and minimal side effects that validate the use of PRT in high-risk neuroblastoma patients, we answered a lingering question about proton therapy – the concern that because it is so targeted, tumors may come back. Tumors mostly did not come back, suggesting PRT is effective, less toxic and a superior choice for our young patients who must endure intense treatment modalities in an effort to cure this high-risk cancer.”
MORE: Boy is Cured of Aggressive Cancer Thanks to Stem Cell Treatment Using Donated Umbilical Cord
Neuroblastoma is the most common cancer in infants, accounting for more than 10% of all childhood cancer deaths. Primary neuroblastoma tumors are commonly adrenal tumors, which are very close to the kidney, liver, pancreas and bowel in children, making them hard to treat without harming vital organs in tiny bodies. Treatment usually involves a combination of therapies including chemotherapy, radiation and surgery.
Typically, the 5-year survival rate of high-risk neuroblastoma patients is as low as 40%. Researchers from CHOP studied 45 patients with high-risk neuroblastoma who received PRT at both of their institutions between 2010 and 2015.
Five years after treatment, the longest recorded period of study in the largest cohort of patients to date, researchers observed excellent outcomes, with 82% of patients still alive, and 97% free of a primary site tumor reoccurrence.
CHECK OUT: UCLA Surgeons Develop Simple Spray Gel to Super-Charge Immunity and Prevent Cancer From Returning
Toxicities, or side effects, are measured on a scale from 1 to 5, with 5 being the most severe. No patient observed in the study experienced grade 3 or 4 long-term acute liver or kidney toxicity, with the majority of patients experiencing grade 1 side effects from PRT.
“We’ve showed PRT is not only effective in the treatment of high-risk neuroblastoma, but it also spared damage to the developing liver, kidneys and bowel that may occur in pediatric patients exposed to traditional radiation,” said Hill-Kayser. “While we look forward to longer-range data on these patients 10 years down the road, the excellent outcomes we see here, coupled with the fact the precision proton approach did not increase recurrence rates, support the expanded use of proton therapy in neuroblastoma and other high-risk childhood cancers.”
Furthermore, a study of 125 pediatric patients that was conducted at Northwestern University in November found that proton therapy was associated with improved cognitive function and an increase of roughly 10 IQ points in contrast to traditional radiation. Additional studies have also claimed that proton therapy is less costly than alternative radiation methods.
“A child’s brain is more sensitive to radiation. The radiation can disrupt connections being formed in the white matter and prevent the brain from developing normally,” said lead author Jeffrey Paul Gross, Northwestern University radiation oncology resident. “If we are able to spare healthy portions of the brain from radiation there is a potential for improved long-term cognitive outcomes.”
PRT used against prostate cancer in adults has also resulted in a 5-year survival rate of 93.25%.
With more and more proton therapy clinics opening up across the US, CHOP researchers say that they will be conducting further studies on the efficacy of the treatment against other cancers.
(WATCH the video below)
Treat Your Friends To Some Good News By Sharing It To Social Media…